Black And African American Communities And Mental Health
Overall, mental health conditions occur in Black and African American (B/AA) people in America at about the same or less frequency than in White Americans. However, the historical Black and African American experience in America has and continues to be characterized by trauma and violence more often than for their White counterparts and impacts emotional and mental health of both youth and adults.
Historical dehumanization, oppression, and violence against Black and African American people has evolved into present day racism – structural, institutional, and individual – and cultivates a uniquely mistrustful and less affluent community experience, characterized by a myriad of disparities including inadequate access to and delivery of care in the health system. Processing and dealing with layers of individual trauma on top of new mass traumas from COVID-19 (uncertainty, isolation, grief from financial or human losses), police brutality and its fetishization in news media, and divisive political rhetoric adds compounding layers of complexity for individuals to responsibly manage.
Help-seeking behavior is affected by mistrust of the medical system and often begins with faith-based outreach. However, MHA screening data shows that Black and African American people who screen positive for depression self-identify as planning to seek help at higher rates than the general population says they will seek help. Unfortunately, Black and African American providers, who are known to give more appropriate and effective care to Black and African American help-seekers, make up a very small portion of the behavioral health provider workforce (see treatment statistics below). Because of these factors and more, Black and African American people are more likely to experience chronic and persistent, rather than episodic, mental health conditions. Yet, hope for recovery should remain, as light is shed on these issues – and the general public holds accountable policymakers and health systems to evolve better systems which eliminate inequities in mental health services.
Demographics/Societal Issues
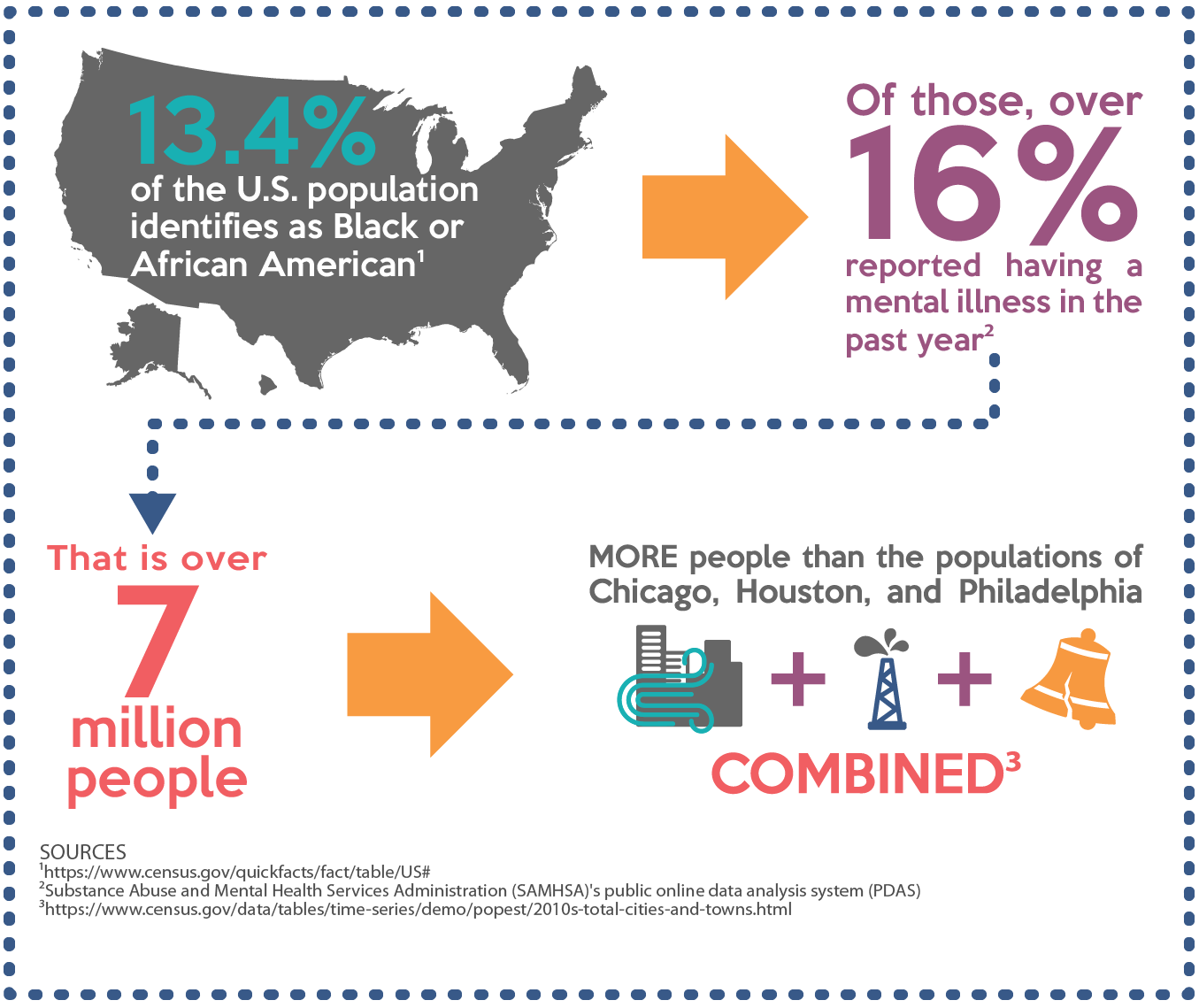
- 13.4 percent of the U.S. population, or nearly 46 million people, identify themselves as Black or African American and another 2.7 percent identified as multiracial. [1]
- According to the most recent Census data available, 55 percent of all Black and African American people lived in the South, 18 percent lived in the Midwest, 17 percent in the Northeast, and 10 percent in the West. [2]
- The Black immigrant population in the U.S. increased from 816,000 in 1980 to over 4.2 million by 2016. Thirty-nine percent were from Africa and nearly half were from the Caribbean. [3]
- Overall, 24 percent of Black and African American people have a bachelor’s degree or higher as of 2017. [3]
- More than 1 in 5 Black and African American people in the U.S. lived in poverty as of 2018. [4]
- Women are the heads of household in roughly 30 percent of Black and African American homes, compared to 9 percent of white homes. [5]
- Historical adversity, which includes slavery, sharecropping, and race-based exclusion from health, educational, social, and economic resources, translates into socioeconomic disparities experienced by Black and African American people today. Socioeconomic status, in turn, is linked to mental health: people who are impoverished, homeless, incarcerated, or have substance use problems are at higher risk for poor mental health.
- Despite progress made over the years, racism continues to have an impact on the mental health of Black and African American people. Negative stereotypes and attitudes of rejection have decreased, but continue to occur with measurable, adverse consequences. Historical and contemporary instances of negative treatment have led to a mistrust of authorities, many of whom are not seen as having the best interests of Black and African Americans in mind.
Prevalence
- Black and African American people living below poverty are twice as likely to report serious psychological distress than those living over 2x the poverty level. [6]
- Adult Blacks and African Americans are more likely to have feelings of sadness, hopelessness, and worthlessness than adult whites. [7]
- Blacks and African Americans are less likely than white people to die from suicide at all ages. [8] However, Black and African American teenagers are more likely to attempt suicide than White teenagers (9.8 percent v. 6.1 percent). [9]
According to SAMHSA’s 2018 National Survey on Drug Use and Health [10]:
- Sixteen percent (4.8 million) of Black and African American people reported having a mental illness, and 22.4 percent of those (1.1 million people) reported a serious mental illness over the past year.
- Serious mental illness (SMI) rose among all ages of Black and African American people between 2008 and 2018.
- Despite rates being less than the overall U.S. population, major depressive episodes increased from 9 percent-10.3 percent in Black and African American youth ages 12-17, 6.1 percent to 9.4 percent in young adults 18-25, and 5.7 percent to 6.3 percent in the 26-49 age range between 2015 and 2018.
- Suicidal thoughts, plans, and attempts are also rising among Black and African American young adults. While still lower than the overall U.S. population aged 18-25, 9.5 percent (439,000) of Black and African American 18-25-year-olds had serious thoughts of suicide in 2018, compared to 6 percent (277,000) in 2008. 3.6 percent (166,000) made a plan in 2018, compared to 2.1 percent (96,000) in 2008, and 2.4 percent (111,000) made an attempt in 2018, compared to 1.5 percent (70,000) in 2008.
- Binge drinking, smoking (cigarettes and marijuana), illicit drug use and prescription pain reliever misuse are more frequent among Black and African American adults with mental illnesses.
Attitudes
According to a study conducted by Ward, Wiltshire, Detry, and Brown in 2013 [11]:
- Black and African American hold beliefs related to stigma, psychological openness, and help-seeking, which in turn affects their coping behaviors. The participants in this study were not very open to acknowledging psychological problems, but they were somewhat open to seek mental health services.
- Thirty percent of participants reported having a mental illness or receiving treatment for a mental illness
- Black and African American men are particularly concerned about stigma.
- Cohort effects, exposure to mental illness, and increased knowledge of mental illness are factors that could potentially change beliefs about symptoms of mental illness.
- Participants appeared apprehensive about seeking professional help for mental health issues, which is consistent with previous research. However, participants were willing to seek out some form of help.
Treatment Issues
- Black and African American people are more often diagnosed with schizophrenia and less often diagnosed with mood disorders compared to white people with the same symptoms. Additionally, they are offered medication or therapy at the lower rates than the general population. [5]
- Black and African American people are over-represented in our jails and prisons. Black and African American people make up 13 percent of the general U.S. population, but nearly 40 percent of the prison population. [12] In 2016, the imprisonment rate for Black and African American men (2,417 per 100,000 Black male residents) was more than 6 times greater than that for white men (401 per 100,000 white male residents) and the imprisonment rate for Black and African American women (97 per 100,000 Black and African American female residents) was almost double that for white women (49 per 100,000 white female residents). [13] Black and African American people with mental health conditions, specifically those involving psychosis, are more likely to be in jail or prison than people of other races. [5]
- Because less than 2 percent of American Psychological Association members are Black or African American, some may worry that mental health care practitioners are not culturally competent enough to treat their specific issues. [14]
- Stigma and judgment prevent Black and African American people from seeking treatment for their mental illnesses. Research indicates that Blacks and African Americans believe that mild depression or anxiety would be considered “crazy” in their social circles. Furthermore, many believe that discussions about mental illness would not be appropriate even among family. [15]
Access/Insurance
Disparities in access to care and treatment for Black and African American people have also persisted over time.
- While the implementation of the Affordable Care Act has helped to close the gap in uninsured individuals, 11.5 percent of Black and African Americans, versus 7.5 percent of white Americans were still uninsured in 2018. [16]
- In 2018, 58.2 percent of Black and African American young adults 18-25 and 50.1 percent of adults 26-49 with serious mental illness did NOT receive treatment. [7]
- Nearly 90 percent of Black and African American people over the age of 12 with a substance use disorder did NOT receive treatment. [7]
- In 2016, 12.3 percent of Black and African American adults who had a doctor’s office or clinic visit over the past year had difficulty getting needed care, tests or treatment compared to 6.8 percent of white adults. [17]
Mental disorders affect nearly 20 percent of American adults; nearly 4 percent are severely impaired and classified as having serious mental illness. These disorders are often associated with chronic physical illnesses such as heart disease and diabetes. They also increase the risk of physical injury and death through accidents, violence, and suicide.
Suicide alone was responsible for 42,773 deaths in the United States in 2014 (the last year for which final data are available), making it the 10th leading cause of death. Among adolescents and young adults, suicide is responsible for more deaths than the combination of cancer, heart disease, congenital anomalies, respiratory disease, influenza, pneumonia, stroke, meningitis, septicemia, HIV, diabetes, anemia, and kidney and liver disease.
The treatment of mental illness has long been held back by the sense that disorders of emotion, thinking, and behavior somehow lack legitimacy and instead reflect individual weakness or poor life choices. Not surprisingly, there has been a mismatch between the enormous impact of mental illness and addiction on the public’s health and our society’s limited commitment to addressing these problems. Here are three examples of how that plays out:
- Most emergency departments are ill-equipped to meet the needs of patients in the midst of mental health crises.
- Most insurance plans view mental illness and addiction as exceptions to standard care, not part of it.
- Despite an overall cultural shift towards compassion, our society still tends to view the mentally ill and those with addiction as morally broken rather than as ill.
Why the disconnect? Psychiatry has been hampered by an inability to observe and record the physical workings of the brain. Because of that, psychiatric assessments and treatments have been viewed as somewhat mysterious. Even today, the underlying mechanisms behind some of the most powerful and effective psychiatric treatments are still poorly understood. All of that translates into the difficulty that many people have finding help for real, disabling symptoms attributed to a mental illness or addiction.
However, just as other fields of medicine have evolved as knowledge advanced during the past century, psychiatry has also made profound gains. Advances emerging from unlocking the brain’s physiology and biochemistry are coming at a time when mental health care is being integrated into traditional health care. The potential has never been greater to finally bring psychiatry quite literally under the same roof as the rest of medicine.Today, the hospital can address mental health issues as effectively as it treats trauma or cardiac arrest. This shift is occurring nationally, with community-involved, comprehensive mental health integration into hospitals in cities and rural communities alike.
Will the stigma of mental illness finally fade? Better understanding of the human brain and the biological nature of the mind will help, but it won’t be enough. How we think about mental health matters. When mental health is ultimately recognized as essential to physical health, not an extraneous element of it, then we will have access to true, complete, modern medicine.
John V. Campo, MD, is professor and chair of the Department of Psychiatry and Behavioral Health at The Ohio State University Wexner Medical Center in Columbus, Ohio.